Key Takeaways from RX Summit
Key Takeaways from RX Summit
Last month leaders from across the US gathered and addressed the opioid epidemic at the 2023 RX Summit.
The yearly conference allowed peer recovery specialists, harm reduction coordinators, social workers, clinical professionals, and administrators to learn about strategies implemented by a variety of organizations in the previous 12 months.
While attendees and speakers shared an array of information about their efforts to combat the epidemic, there was a common theme: what we’ve been doing is not enough. Federal partners and local leaders are looking for new ways to treat, prevent, and educate their communities about substance use disorder (SUD), but several challenges persist:
Opposing views about Medication Assisted Treatment vs. Sobriety
Treatment with MAT (medication assisted treatment) runs counter to the notion of abstinence and sobriety. The change in position on the use of mental health medication for people diagnosed with depression or anxiety has impacted many treatment facilities that require absolute abstinence. Unfortunately, many of the medications that are used for the treatment of mental health issues are also medications that can be misused or abused. The risk of allowing those medications in a sober living house is too risky for the rest of the community. The tension between the two perspectives means that some people are not getting the care they need. In fact, at a recent datathon focused on maternal mortality, a team was able to show that some new mothers are not given the postpartum care they need because they stop their medication for pregnancy and do not return to MAT or mental health medications.

The Need to Update Our Understanding of Adverse Childhood Events
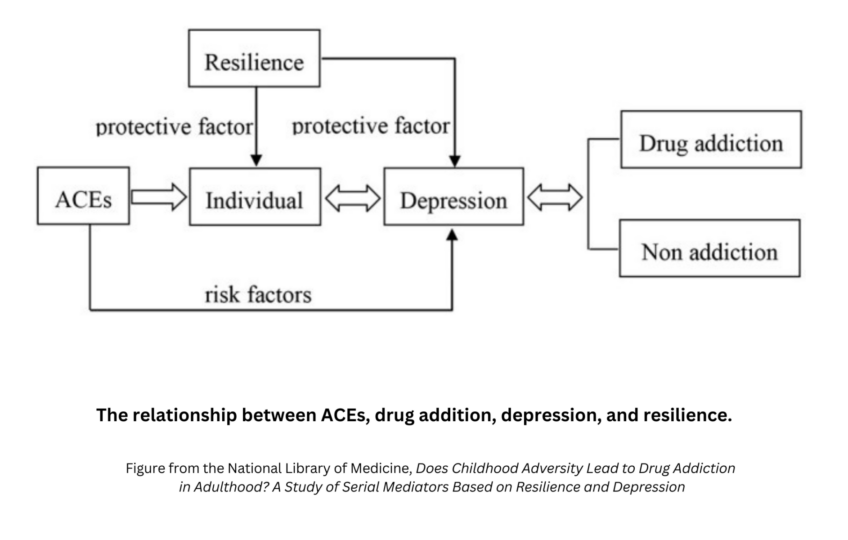
Adverse Childhood Events (ACEs) are a critical area of focus in the prevention of substance use disorders and addiction. Research shows a positive correlation between ACEs and addiction, mental health problems, and other negative health outcomes later in life. Historically, the treatment community has defined ACEs as traumatic experiences related to abuse, neglect, and household challenges like homelessness. However, recent data shows that many young people who have not experienced any ACEs are using opioids. Leaders from across the healthcare community are pointing out that the research on ACEs might need to be updated to address the impact of social media on the mental health of a teen, for example.
Stigma Around Addiction Continues to Hinder Education and Awareness
A growing body of research suggests that stigma reduces the likelihood of policymakers to allocate resources to treatment programs, decreases the chances that providers screen for SUD-related issues, and limits the willingness of individuals to seek treatment. It’s imperative that we continue to educate the public—especially healthcare and social services workers, parents, and educators—about the reality of substance use disorder: that it’s a disease, not a character flaw.
How Data and Analytics Can Help
Effectively addressing the root causes of the opioid epidemic involves addressing a pervasive information management issue. The information available currently is incomplete, disjointed, and often not actionable, making it difficult to fully understand the nature of the crisis and devise appropriate policy measures. Additionally, the lack of comprehensive and coherent data makes it challenging to motivate physicians and patients to engage in behaviors that can help mitigate the crisis.
Despite the considerable difficulty of managing information related to the opioid epidemic, it is crucial that we continue to increase our efforts towards gathering, organizing, and utilizing available data to generate actionable insights through analytical tools. With a constantly evolving problem that varies from community to community, it is critical that solutions implemented are scalable, local, and usable by all stakeholders, including front-line workers, local leaders, healthcare providers, public safety personnel, and policymakers.

During the RX Summit, a Virginia Department of Criminal Justice representative and Voyatek’s Lyd Paull-Flores demonstrated how data and analytics has facilitated Virginia’s response to the opioid epidemic. Virginia’s Framework for Addiction Analysis and Community Transformation (FAACT), developed by Voyatek in partnership with DCJS, has delivered important outcomes across the commonwealth. Virginia has:
Slowed the growth rate of Fentanyl overdose deaths; Virginia is now in the bottom 40% of states with the 2022 results showing a statistically significant decrease in the number of fatal cases.
Launched a new prevention and outreach program to educate younger children and their parents after Voyatek’s analytics identified the self-reported of age of first use to be 12 years old, much younger than previously reported.
Enabled real-time overdose spike alerts for local community service providers and first responders. For example, FAACT identified an unexpected spike in a certain veterinary medicine (xylazine) being mixed with opioids. A provider alert was quickly issued by the Department of Behavioral Health and Developmental Services, the Office of the Chief Medical Examiner, and the Virginia Department of Medical Assistance Services (Virginia Medicaid) so that front-line providers could be on the lookout when treating patients. By coordinating with local opioid coalitions, Virginia was able to get a head start on addressing Xylazine usage before national alerts from CDC and FDA were released.
Identified and prioritized local substance use treatment needs after the system produced the first comprehensive resource map displaying where overdoses occur compared to existing treatment facilities allowing the community in South-Western Virginia to pilot a Narcan Vending machine to increase the Narcan distribution footprint as part of their SOR funded activities.
Assisted localities in being awarded $1M in SAMSHA funding that allows for therapeutic care to be delivered in the high schools for young people who struggle with SUD or experience an overdose and offering their family wrap around services rather than being removed from their community, and from their family’s care, and sent to an inpatient setting.
-Voyatek Leadership Team

